Functional Rhinoplasty in Virginia, Washington D.C. and Maryland.
Embark on a journey of aesthetic excellence with The Naderi Center. Experience unparalleled artistry and precision for transformative beauty.
Discover Functional Rhinoplasty Benefits
Discover the transformative advantages of Functional Rhinoplasty. This specialized procedure not only addresses aesthetic concerns but also significantly improves your breathing. Engineered for those who seek a dual solution for cosmetic and functional issues, Functional Rhinoplasty offers multiple benefits that go beyond surface-level changes.
Enhanced Breathing
Experience immediate relief from nasal congestion or obstruction. Say goodbye to sleepless nights and hello to unrestricted airflow.
Balanced Aesthetics
Achieve a harmonious facial symmetry with subtle refinements that complement your natural features, all without compromising function.
Faster Recovery
Unlike traditional procedures, Functional Rhinoplasty ensures a quicker healing process, allowing you to enjoy your new look and improved breathing sooner.



Types of Functional Rhinoplasty
Explore the versatile world of Functional Rhinoplasty types designed to address various concerns. Whether you’re dealing with breathing issues or seeking subtle aesthetic changes, there’s a tailored solution for you. These specialized types of Functional Rhinoplasty offer targeted corrections to meet your unique needs, delivering both cosmetic and functional benefits.
Nasal Fracture (Broken Nose) Repair
The nasal bones are amongst some of the weakest bones in the body. The nasal cartilages at the bottom 2/3rd of the nose are like spring boards or car bumpers to prevent fractures with minor trauma. More severe trauma can break or dislocate the nasal cartilages as well as the nasal bones.
After a nose trauma, the most important step is to make sure other facial bones are not affected such as the cheek and eye socket (orbital) bones. It’s also crucial to be examined to make sure there is no hematoma inside the nose – septal hematoma which is defined as blood collection inside the lining of the septum. This can cause necrosis and death of the septum and nasal collapse or septal perforations (hole in septum). Immediate diagnosis and evacuation of septal hematoma is necessary to prevent this devastating complication of a nasal fracture or trauma.
While CT scans and X-rays are good for diagnosis of other facial bone fractures, the diagnosis of a nasal fracture is a “clinical diagnosis” requiring physical examination and thorough history taking by the Emergency Room doctor.
The nose should be evaluated by a Plastic Surgeon after a few days when the swelling has gone down. Emergency room physicians are usually the initial examining doctors. If a Closed Nasal Reduction is needed to reset the nose back, this should be done between 5 to 12 days after the initial trauma; not too soon so that swelling obscures the contour of the nose and not too late so that the nose has completely set! The other option is for Open Nasal Reduction with osteotomies to rebreak the nasal bones in a more favorable fashion and reduce the nasal fracture. This can be done at any time; however, doing this 5 days post-fracture and prior to 1 month is best. The final treatment is a full Septo-Rhinoplasty to reconstruct the nose. This should be done 3 months after the initial trauma so most of the swelling is gone. A complete septo-rhinoplasty done too early will not have precise results and should be delayed to at least 3 months after the trauma. Most often, insurance will not pay for a complete septo-rhinoplasty while many insurances do pay for Closed Nasal Reduction and/or Open Nasal Reduction. If the nose is extremely damaged, then the procedure may need to be staged with an initial closed or open nasal reduction to improve the nose as best as possible and then a complete septo-rhinoplasty later on to improve on the initial fracture reduction.
Nasal fractures in young children are especially problematic as the nose and septum are important in growth of the mid-face and damage to the growth centers can have adverse effects. This is why plastic surgeons advise on avoiding major septoplasty on children younger than 14 years of age.
Reconstructive Rhinoplasty
The nose is easily susceptible to trauma, dog bites, injury, and skin cancer. While damage to the underlying bone and cartilage can be repaired through a Septo-Rhinoplasty, missing or damaged skin needs to be repaired as well if indicated. Small defects on the nose tip can be repaired by full thickness skin grafts but all other locations on the nose and all larger defects require flaps for reconstruction. Some commonly used flaps are the bilobed flap, the rhomboid flap, the paramedian forehead flap, the melolabial flap and the sliding glabellar flap. Complete defects may require free tissue flaps such as the radial forearm free flap. Underlying structure – if missing – must also be replaced with ear cartilage or rib cartilage, etc. Internal lining of the nose must also be addressed. Therefore, larger nasal defects become an issue of triple layer reconstruction. Dr. Gary C. Burget in Chicago, Illinois and Dr. Frederick J. Menick in Tucson, Arizona, and Dr. Shan Baker in Livonia, Michigan are world famous for large defect nasal reconstructions requiring multiple stage repair.
Septoplasty
While rhinoplasty is most often a cosmetic operation, septoplasty can also have cosmetic benefits and vice versa. A crooked nose is often partially due to a deviated septum and correction of the crooked septum can help straighten out the nose with cosmetic and functional breathing improvements. Conversely, a deviated septum that is also accompanied by a crooked nose may need to be addressed together. Otherwise, simple attempts at correction of the crooked septum without correction of the crooked nose may only be partially effective at correcting the deviated septum – if at all.
The nasal septum is made up of various components of bone and cartilage with connection to the skull base and coverage with mucosal lining on both sides. Not only does the anatomic structure of the septum lead to nasal airway obstruction issues but the health of the mucosal lining itself has a large part in the nasal health and breathing ease of each patient. Allergic rhinitis, inflammation, collagen vascular and auto-immune diseases, cocaine use, infections, trauma, genetically deviated septa, and other causes can lead to nasal airway obstruction.
A facial plastic surgery specialist surgeon who is a facial plastic surgeon with training in both ENT- Head & Neck Surgery as well as Plastic Surgery of the face, head and neck is best equipped to deal with these complex issues. For straight forward septoplasty, most general ENT surgeons do a very fine work.
Nasal Reconstruction
While a nose that looks good brings balance and harmony to the face, it should not be at the sacrifice of breathing. Patent and functional nasal passages are a vital part the nose. The inside of the nose should be as nice as the outside. Often, many Plastic Surgeons have very little to no training on functional nasal surgery so even if they happen to create a cosmetically appealing nose, they may neglect to fix the inside (functionality) or worse, cause more problems with functionality.
The inside of the nose and the outside of the nose are intimately connected. The nasal septum on the inside is the structural wall and foundation of the external nasal architecture. Think of the nose as a building. The septum is the support inner wall while the outside of the nose is roof. You cannot have a straight roof with crooked walls! Therefore, if a naïve Plastic Surgeon fails to recognize or diagnose a deviated septum prior to Rhinoplasty, then he may actually create or worsen the appearance of a crooked nose. The old saying amongst Facial Plastic Surgeons is “Where goes the septum, so goes the nose!”
While the septum provides a source of cartilage for grafts during Rhinoplasty, its own structure is important. A crooked septum often must be straightened during a cosmetic Rhinoplasty. However, not all patients have a deviated septum. Slight deviations are very common and perfectly straight septa are rare. Often, patients wonder if insurance will cover some or all of the Rhinoplasty if there is septal deviation. In most situations, the two parts of the procedure are billed separately. A cosmetic Rhinoplasty is not billed to insurance. Insurance may cover a small portion of the surgeon’s fee as well as part of the anesthesia and hospital fees. Ethically and legally, the cosmetic portion should not be billed to insurance. However, if there is a true and problematic septal deformity, then insurance should hopefully cover that portion of the surgery. Enlarged turbinates may also create nasal airway obstruction. Turbinates are the humidifiers of the nose and they fluctuate in size during the day. They even alternate from side to side in a process called the “nasal cycle.” While the turbinates may be trimmed, they should not be aggressively reduced or completely removed. This type of aggressive turbinate reduction, commonly done in the past, leads to atrophic rhinitis also known as empty nose syndrome. It’s quite a problematic functional internal nasal deformity that is not easily fixable.
Vestibuloplasty, also known as spreader grafts, can widen the internal valve area just above the nasal tip and below the nasal bones and improve nasal airflow. Alarplasty with alar rim grafts or alar batten grafts can provide strength and support to the nostrils and lessen or prevent dynamic inspirational nasal collapse.
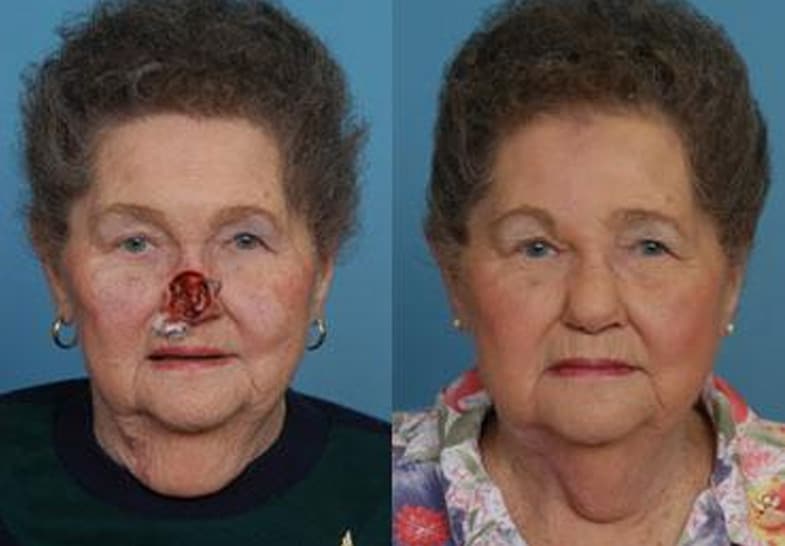
Nasal reconstruction is more for reconstruction of the nose after MOHS skin cancer removal or trauma resulting in nasal tissue loss. Various techniques can be used including local and regional flaps. Some are done in one stage while others may require several surgeries for optimal results.
Turbinate Reduction Virginia
The nasal turbinates are the humidifiers of the nose. There are 3 to 4 turbinates on each side of the nose, opposite to the septum. While the nasal septum is stationary and usually does not move, the nasal turbinates are covered with a vascular spongy lining that engorges and swells up at times and then shrinks down at other times, creating what’s known as “the nasal cycle.” Allergies, crying, laying down, smoke, and other factors can cause the turbinates to swell up further and obstruct the nose especially if the septum is already somewhat deviated.
Since 60% of the nasal airflow typically crosses the bottom part or “floor of the nose,” the inferior (bottom) turbinates are the ones that often benefit from reduction. The key is reduction and not complete removal of the turbinates because they are important in nasal health and humidification and total removal or over aggressive turbinate reduction can lead to a horrible and crippling problem known as “atrophic rhinitis” or “empty nose syndrome.”
Functional Rhinoplasty FAQs
Who is an ideal candidate for functional rhinoplasty?
An ideal candidate for functional rhinoplasty is someone experiencing breathing difficulties due to nasal structural issues, such as a deviated septum, nasal valve collapse, or chronic nasal obstruction. Good health and realistic expectations are also important.
What should I expect during a functional rhinoplasty consultation?
During the consultation, your surgeon will evaluate your nasal structure, discuss your breathing issues, and review your medical history. They may use imaging studies to plan the surgery and explain the potential outcomes and recovery process.
How is functional rhinoplasty different from cosmetic rhinoplasty?
Functional rhinoplasty focuses on improving nasal function and breathing, while cosmetic rhinoplasty primarily aims to enhance the nose's appearance. Both procedures can be combined if the patient desires both functional and aesthetic improvements.
How long is the recovery period after functional rhinoplasty?
The initial recovery period typically lasts about 1 to 2 weeks, during which swelling and bruising subside. Full recovery and final results can take up to a year as the nasal tissues heal and settle into their new structure.
Are there any risks associated with functional rhinoplasty?
Risks include infection, bleeding, scarring, and dissatisfaction with the results. However, choosing an experienced surgeon can significantly minimize these risks and ensure a successful outcome. Discuss potential risks thoroughly with your surgeon.
How should I prepare for a functional rhinoplasty procedure?
Preparation includes avoiding smoking, discontinuing certain medications, and following your surgeon's specific pre-operative instructions. Proper preparation can help ensure a smoother surgery and recovery process.
Can functional rhinoplasty be combined with other procedures?
Yes, functional rhinoplasty can be combined with cosmetic rhinoplasty or other facial procedures to address both functional and aesthetic concerns. Your surgeon can create a comprehensive treatment plan tailored to your needs.
What is the typical cost of a functional rhinoplasty procedure?
The cost of functional rhinoplasty varies based on factors such as the surgeon’s expertise, the complexity of the procedure, and the facility’s location. For an accurate estimate, consult with a qualified healthcare professional.
How soon will I see results after functional rhinoplasty?
Improvement in breathing is often noticeable soon after the procedure, but swelling may temporarily affect the final appearance. Most patients see significant functional improvements within a few weeks, with full results becoming apparent after several months.
Is functional rhinoplasty covered by insurance?
Functional rhinoplasty may be covered by insurance if it is deemed medically necessary to correct breathing problems. It is important to check with your insurance provider and surgeon's office to understand coverage and any out-of-pocket costs.